A Call for Policies and Regulations to Strengthen Antimicrobial Stewardship
By Kate Kikule and Niranjan Konduri, USAID MTaPS
Ensuring the appropriate use of antimicrobials
Bacterial infections are a significant problem across the human and animal worlds and accelerate the consumption of antimicrobial medicines. In OECD countries where data exist, it is seen that only half of antimicrobial consumption is by humans, mainly in oral dosage forms; the rest are mainly added to food for animals (pigs and poultry in particular) for mass treatment of infectious diseases or to promote growth. Laws, policies, regulations, and guidelines are needed to ensure appropriate use, avert inappropriate prescribing and dispensing practices, and deter self-medication. However, many low- and middle-income countries lack restrictions on prescribing antimicrobials, which accelerates indiscriminate use across the human, animal, and agricultural sectors. In many countries, overuse and misuse is a consequence of direct purchase from medicine shops, insufficient knowledge, promotion of medicines, and profit motivation—all of which is driving antimicrobial resistance (AMR).
Reducing AMR and ensuring appropriate use across countries depends on the implementation of global strategies and recommended regulations by all nations on five continents in the human, animal, fisheries, veterinary, and environmental health sectors. For rules to be enforced and effective, national regulatory authorities should be equipped and adequately funded by the government or other sources to effectively control medicines and related practices.
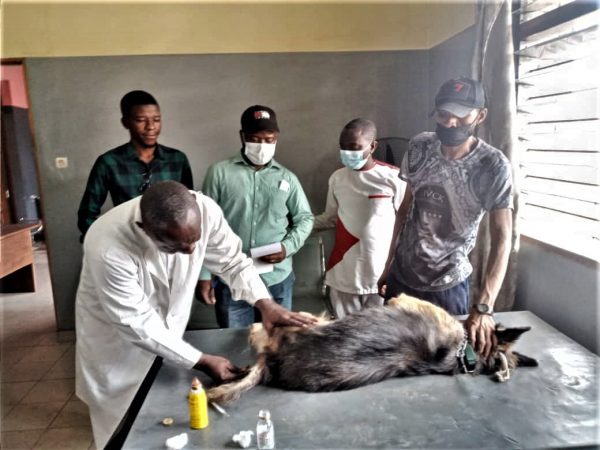
A sick dog under consultation at a veterinary clinic in Kinshasa, DRC. Photo credit: Tatiana Banze, MTaPS DRC
The WHO Benchmarks for International Health Regulations Capacities for AMR emphasize the need for countries to assess current laws, regulations, policies, and administrative guidelines governing the management and regulation of antimicrobials in both the human and animal health sectors. Benchmark 3.4 on optimizing the use of antimicrobials in human and animal health and agriculture recommends that domestic legislation, laws, regulations, policy, and administrative requirements be available in all relevant sectors and enable compliance with the International Health Regulations.
Examples from three countries
The USAID Medicines, Technologies, and Pharmaceutical Services (MTaPS) Program supported several countries in Africa to perform a rapid assessment of stewardship policies and activities, including a regulatory framework to identify salient gaps that need to be addressed in the human and animal sectors using a multisectoral approach. We found that in Burkina Faso, Mozambique, and Uganda there is inadequate control of the veterinary sector, which is manifested by weak implementation and enforcement of regional regulations to manage the animal health sector. The prevalence of inappropriate use of antimicrobials in the veterinary sector, such as direct sale by distributors to farmers, is against good distribution practices guidelines. This is consistent with the OIE finding that 70% of responding countries in the African region reported not having any legislation or regulation banning the use of critically important antimicrobials in the animal health sector. On the other hand, legislation governing the use of antimicrobials in human health exists in these three countries. However, appropriate guidelines and reporting systems on their use and surveillance remain a problem due to limitations in health practices and inadequate resources and accountability systems. This is consistent with a recent global survey by WHO, FAO, and OIE (the “Tripartite”), which found that only 33% of countries have guidelines and practices to optimize the use of antimicrobials that are being implemented nationwide in most health facilities, with surveillance results used to update treatment guidelines and essential medicines lists.
A call to action to strengthen multisectoral antimicrobial stewardship policies, regulations, and guidelines
The human, animal, fishery, and agricultural sectors must address key institutional gaps that hinder effective antimicrobial regulation—namely market authorization, regulatory inspections, licensing of premises, post-market surveillance, and pharmacovigilance. This is in line with international standards and recommendations, such as those by FAO, OIE, and WHO.
Other essential areas that need urgent attention include:
- Policies and regulations for prescribing and use of antimicrobials in the human health sector to promote their appropriate use (e.g., legislation on ‘prescription only’ sales of antibiotics)
- Policies to promote appropriate prescribing and utilization of veterinary medicines to avoid the surge of AMR pathogens that can adversely affect human, animal, and environmental health
- Support for diagnostic laboratory infrastructure and practices to promote appropriate administration of treatments
- Strengthening veterinary services, including capacity building of veterinary health providers and experts in appropriate use of antimicrobials, through training with illustrative information, education, and communication materials
- Inclusion of antimicrobial stewardship content in university curricula for training veterinarians and fish health specialists for safe disposal of antimicrobials at the farm level to protect the environment
- Establishment of adequately funded and effective enforcement mechanisms together with post-market surveillance and pharmacovigilance as part of regulatory oversight
In conclusion, the creation and enforcement of robust policies and regulatory framework is needed to strengthen and improve antimicrobial stewardship for both the human and animal sectors at the national and regional levels.